Have you ever wondered if there are infection risks in the healthcare setting? In the realm of modern healthcare, the facilities we trust to heal can sometimes inadvertently become sources of illness. One of the primary culprits? Healthcare-associated infections, or HCAIs.
These infections, which patients acquire while receiving medical treatment, pose significant challenges not only for affected individuals but also for healthcare professionals and institutions.
By diving deep into the world of HCAIs, we can understand their origins, learn about the common pathogens involved, and most importantly, devise strategies to mitigate their risks. A proactive approach can ensure the safety of both patients and healthcare workers.
Understanding Healthcare-Associated Infections (HCAIs)
HCAIs, commonly referred to as nosocomial infections, are infections that weren’t present or incubating in the patient when they entered a healthcare setting but developed 48 hours or more after admittance.
Examples include surgical site infections after operations, urinary tract infections due to catheter use, and respiratory infections from ventilators.
Common Culprits Behind HCAIs
Many microorganisms can lead to HCAIs. However, some bacteria and viruses emerge as frequent offenders. Bacteria like Staphylococcus aureus (including MRSA), Escherichia coli, and Pseudomonas aeruginosa are notorious for causing infections in hospital settings. Viruses such as the influenza virus, norovirus, and occasionally, coronaviruses can also lead to outbreaks within healthcare facilities.
Key Sources of Infection in a Healthcare Setting
- Direct Contact:
In a healthcare environment, the most straightforward transmission route is direct contact. This can occur in various ways, such as:
- Patient-to-patient: In shared rooms or common areas, patients can transmit infections to each other.
- Patient-to-healthcare worker: An infected patient can transfer the infection to a doctor, nurse, or other healthcare staff.
- Healthcare worker-to-patient: In the absence of proper hygiene and precautions, staff can transmit infections to patients.
- Medical Instruments and Equipment:
Inadequate sterilization or cleaning can turn life-saving tools into potential threats. Reusable instruments like endoscopes or surgical tools, if not properly sanitized, can introduce infections. Similarly, contaminated single-use items like syringes can also pose risks. - Airborne Transmission:
Certain diseases, like tuberculosis or influenza, can spread through the air. In areas like operating rooms or isolation wards, poor ventilation or lack of proper air filtration systems can facilitate the spread of airborne pathogens.
Most Vulnerable Areas Within Healthcare Facilities
Healthcare settings, designed with the intention to heal, unfortunately, can also be breeding grounds for infections if not vigilantly managed.
Certain areas within these facilities are particularly susceptible due to the nature of treatments, the condition of the patients, and the intricacies of the equipment used. Let’s delve into some of the most vulnerable areas:
- Intensive Care Units (ICUs)
ICUs cater to critically ill patients requiring close monitoring and support. These patients often have compromised immune systems, making them more susceptible to infections.
Prolonged hospital stays, the necessity of multiple medical devices, and constant interaction with healthcare staff further increase the potential for acquiring HCAIs in ICUs.
- Operating Rooms
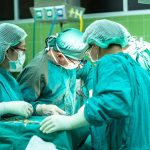
Though stringent sterilization protocols are maintained in operating rooms, they remain vulnerable to infections. Surgical site infections can occur if pathogens are introduced during surgery, either from non-sterile instruments, the external environment, or even the patient’s own skin flora. - Neonatal Units
Neonatal units, or neonatal intensive care units (NICUs), are designed for the care of premature or critically ill newborns. Given the underdeveloped immune systems of these infants, even common microbes can pose severe threats. - Dialysis Centers
Patients undergoing dialysis often have weakened immune systems due to chronic kidney disease, making them more susceptible to infections.
The process of dialysis, especially hemodialysis, involves accessing the bloodstream, providing a direct route for pathogens if not handled with extreme care.
Contaminated dialysis machines, water supplies, or even minor lapses in hygiene can lead to serious infections, including bloodstream infections.
High-Risk Procedures and Interventions
While healthcare facilities provide life-saving treatments, certain procedures inherently carry a higher risk of infection due to their invasiveness, complexity, or the areas of the body they involve.
Understanding these risks can lead to more informed decisions and enhanced preventative measures. Let’s explore some of the high-risk procedures and interventions:
Surgery
Whenever the body’s natural barriers are breached, such as in surgical procedures, there’s potential for pathogens to enter.
While operating rooms have strict sterilization protocols, surgeries—particularly those that are lengthy or complex—can still introduce risks.
Factors that can contribute to surgical site infections include the surgical environment’s cleanliness, the sterilization of instruments, the health and hygiene of the surgical team, and even the patient’s own health and nutritional status.
Catheter and Tube Insertions
Catheters, tubes, and other inserted medical devices play crucial roles in monitoring and treating patients.
However, their insertion points can serve as entry gates for bacteria if not properly cared for. Urinary tract infections from urinary catheters or bloodstream infections from central venous catheters are examples.
Regular inspection of insertion sites, strict hygiene during insertion and removal, and timely removal of these devices when no longer necessary can mitigate these risks.
Ventilation
Mechanical ventilation is life-saving for patients who can’t breathe independently. However, it comes with risks. Ventilator-associated pneumonia (VAP) is a primary concern, arising from the introduction or buildup of pathogens in the respiratory system.
Preventing VAP involves strategies such as maintaining proper hygiene when handling ventilation equipment, regularly suctioning secretions, and elevating the head of the patient’s bed to reduce aspiration risks.
Dialysis
Dialysis, specifically hemodialysis, involves cleaning the patient’s blood outside of their body. As this process necessitates direct access to the bloodstream, it poses a significant infection risk.
Importance of Hand Hygiene
In the sprawling landscape of healthcare and infection control, one might be surprised to learn that one of the most straightforward practices holds paramount importance: hand hygiene.
From the household to the hospital, the simple act of washing hands can have profound effects on health outcomes. Let’s delve deeper into why this basic measure is so significant.
Role of Hand Hygiene in Preventing Infections
Hands are the primary conduits of germ transmission. Healthcare workers move from patient to patient, touch various surfaces, and handle equipment.
Without proper hand hygiene, pathogens can easily spread, leading to potentially serious infections.
In fact, the World Health Organization (WHO) has identified hand hygiene as the single most important practice in reducing the spread of antimicrobial-resistant organisms and healthcare-associated infections.
Proper Handwashing Techniques
Simply running hands under water isn’t enough. Effective handwashing involves several crucial steps:
- Wetting hands with clean running water (warm or cold).
- Applying soap generously.
- Rubbing hands together to create a lather, ensuring coverage of the back of hands, between fingers, and under nails.
- Scrubbing for at least 20 seconds (humming the “Happy Birthday” song twice is a popular timing technique).
- Rinsing hands thoroughly under clean running water.
- Drying hands with a clean towel or air dryer.
Hand Sanitizers vs. Soap and Water
While hand sanitizers offer convenience, especially when soap and water aren’t readily available, they’re not a universal replacement.
Sanitizers with at least 60% alcohol can quickly reduce the number of microbes on hands in many situations, but they don’t eliminate all types of germs.
Soap and water are more effective against certain pathogens, like norovirus and Cryptosporidium.
Strategies to Mitigate Infection Risks
These strategies, when applied holistically, can dramatically reduce the risks associated with infections in healthcare settings.
Regular Training and Education
Healthcare workers should undergo regular training sessions to stay updated on the latest infection control protocols.
This includes understanding the modes of transmission, recognizing early signs of infection, and knowing the steps to take when an outbreak occurs. A well-informed team is a vital first line of defense against infections.
Environmental Cleaning and Sterilization
Maintaining a clean environment is paramount. Regularly disinfecting surfaces, especially high-touch areas like doorknobs, bed rails, and medical equipment, can limit the spread of pathogens.
Surveillance and Monitoring
Hospitals should have surveillance systems in place to monitor and track infection patterns.
By analyzing data and recognizing trends, it becomes easier to predict potential outbreaks and take preemptive measures.
Regular audits can also ensure that infection control measures are being consistently and effectively implemented.
- Isolation Protocols
Patients showing signs of contagious infections should be isolated to prevent the spread to others. This includes having designated isolation wards, utilizing protective barriers like masks and gloves, and ensuring that healthcare workers interacting with these patients follow strict protective measures.
- Antibiotic Stewardship
The overuse of antibiotics can lead to antibiotic-resistant bacteria. It’s essential to use these drugs judiciously.
An antibiotic stewardship program ensures that patients receive the right antibiotic, at the right dose, and for the right duration, helping to combat the rise of antibiotic-resistant infections.
- Patient Education
Patients and their families should be educated on the importance of hygiene, recognizing signs of infections, and following post-operative or treatment care instructions.
An informed patient can actively participate in their care, further reducing the risk of infections.
- Vaccination Programs
Vaccines are a powerful tool in preventing the spread of infectious diseases. Healthcare facilities should promote and provide vaccination programs for both staff and patients, targeting diseases prevalent in the community or specific to the healthcare setting.
The Role of Technology in Preventing HCAIs
In the dynamic world of healthcare, technology has consistently emerged as a beacon of innovation, driving advancements that dramatically impact patient care.
Its role in preventing Healthcare-Associated Infections (HCAIs) has become especially pivotal, as institutions globally harness technology’s potential to enhance safety and reduce infection risks. Here’s a closer look at how technology is reshaping the landscape of infection prevention.
Electronic Health Records (EHRs)
EHRs facilitate seamless sharing and updating of patient information. With real-time updates, healthcare providers can swiftly identify potential outbreaks, track patients’ exposure to infectious agents, and monitor adherence to infection control protocols.
Automated Surveillance Systems
Advanced surveillance systems can automatically detect and alert healthcare teams about unusual patterns or spikes in infections. This rapid detection aids in quicker responses, timely interventions, and reduced spread of HCAIs.
UV Light Disinfection
Ultraviolet (UV) light robots can be deployed in hospital rooms and ORs to eliminate pathogens on surfaces. These robots reduce the reliance on manual cleaning and ensure a higher degree of sterilization, effectively lowering infection risks.
Telemedicine
By leveraging telemedicine for consultations, especially in infectious cases, direct contact and potential spread of infections can be minimized. This protects both patients and healthcare workers.
AI and Machine Learning
AI-driven algorithms can analyze vast amounts of data to predict potential outbreaks, identify at-risk patients, and recommend customized infection control measures. By forecasting and proactively addressing risks, the spread of HCAIs can be dramatically reduced.
Wearable Patient Monitors
Wearable devices can continuously monitor patients’ vitals and detect early signs of infections. Early detection means faster intervention and potentially better outcomes.
Smart Sensors and IoT
Smart sensors, when integrated into the healthcare infrastructure, can monitor and ensure that hand hygiene protocols are being followed. For instance, sensors on soap dispensers can record usage and alert staff if handwashing rates are below set standards.
Drone Technology
Drones can be used to deliver medical supplies, especially in quarantine zones, reducing the need for human contact and thereby reducing the risk of spreading infections.
Antimicrobial Touchscreens and Keyboards
As touchscreens and keyboards are high-touch areas, using ones with antimicrobial coatings can significantly reduce the spread of pathogens.
Virtual Reality (VR) Training
VR can be used to train healthcare workers in infection control practices, allowing them to practice in a simulated environment before applying skills in real-life settings.
My final thought on infection risks in the healthcare setting
As we’ve journeyed through the intricate facets of Healthcare-Associated Infections (HCAIs) and their prevention, one truth remains unequivocal: the importance of collective awareness and proactive measures cannot be overstated.
HCAIs, while being a substantial challenge in healthcare settings, are not insurmountable. The key lies in understanding the risks, acknowledging the gravity, and adopting the best practices and innovations tailored to combat them.
The role of healthcare professionals is, undoubtedly, central in this endeavor. Still, it’s essential to realize that combating HCAIs is not a solitary battle.
It’s a collaborative effort that necessitates the involvement of everyone— from the dedicated nurse on the hospital floor to the patient seeking care, and from the meticulous administrator ensuring protocol adherence to the janitorial staff maintaining cleanliness.
The synergy of this collaboration, fueled by knowledge and guided by best practices, will form the foundation upon which safer healthcare environments are built. It’s an ongoing commitment, one that demands vigilance, continuous learning, and mutual respect.
Editor’s Picks
Prevention Of Blood Loss And Blood Transfusion In Surgery
Effects of substance abuse on individual family and community
4 Types Of Rehabilitation And When Each Is Needed
Top 10 Substance Abuse Nurse Certification Programs